WINNIPEG -- Hope is on the horizon for the COVID-19 pandemic.
The first doses of the Pfizer-BioNTech vaccine were administered on Wednesday, with a total of 900 health-care workers receiving the first of two doses by the end of the week.
While it will take until 2021 until more Manitobans can be vaccinated, those on the front lines are looking at the way the health-care system is currently being impacted, and what changes could be coming in the future.

A red (COVID-19 positive) intensive care unit at the Health Sciences Centre in Winnipeg on Tuesday, Dec. 8, 2020. (MIKAELA MACKENZIE / WINNIPEG FREE PRESS)
'WE EXPECT OUTBREAKS TO OCCUR'
On Oct. 30, 2020, Manitoba reported a then-record 480 new cases of COVID-19. Since that day, the total daily number of reported cases has not fallen below 100, with the highest number of cases in one day being reported on November 23, with 543 new cases.
Health officials say the high daily case counts have placed a strain on the system, which in turn is leading to issues in care.
One of the issues that has emerged throughout the pandemic is COVID-19 outbreaks in hospitals. Several hospital units in Winnipeg, including the Health Sciences Centre (HSC), have dealt with outbreaks in units.
“We expect outbreaks to occur,” said Dr. John Embil, medical director of infection prevention control at the HSC, “It's a given. It's the reality of providing care in a pandemic. So we've got a whole bunch of contingencies in place.”
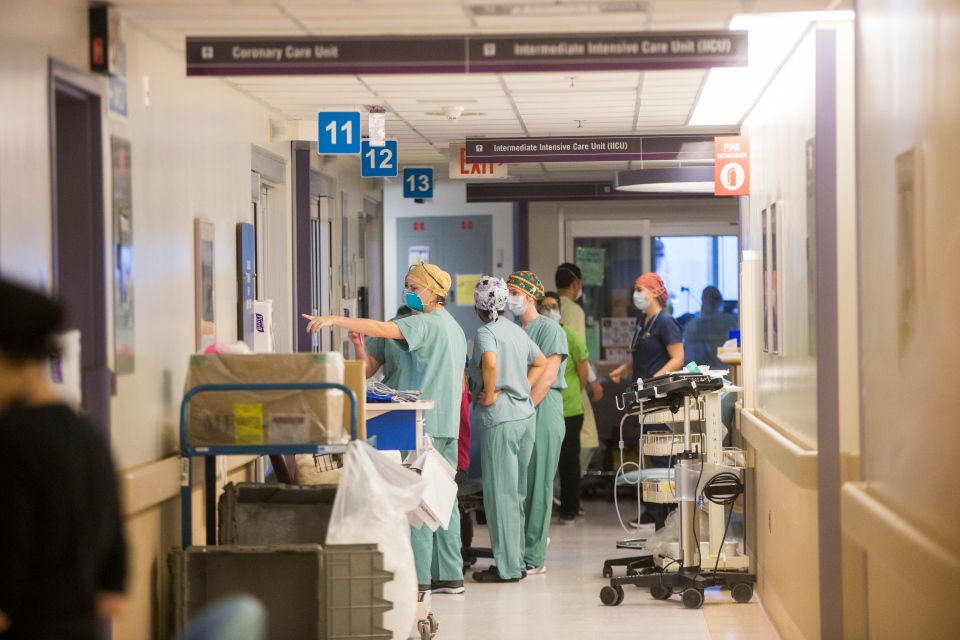
The medical intensive care unit at the Health Sciences Centre in Winnipeg on Tuesday, Dec. 8, 2020. (MIKAELA MACKENZIE / WINNIPEG FREE PRESS)
Some of the contingencies include transferring patients to a new unit, including the former women’s hospital, due to the private rooms there.
Embil added despite the best efforts, outbreaks will still happen.
“Despite our best screening measures, patients will still be incubating germs when they come to hospital,” he said. “We can screen them with the laboratory test (but) that test only gives you a result that's meaningful, the minute the test was taken.”
'THERE'S NOTHING MORE THE HOSPITAL SYSTEM CAN DO'
Dr. Bojan Paunovic, the site director for critical care at the HSC, said staff at four different hospitals are managing 120 critical care beds, and the level is not sustainable if cases continue to rise.
“The concern is to keep going beyond that, or to sustain what we're doing long-term is not something that we should be counting on,” Paunovic said. “We should be counting on the case numbers dropping so that we can continue to provide the care that we've been providing to this point.”

An operating room in the empty day surgery unit at the Health Sciences Centre in Winnipeg on Tuesday, Dec. 8, 2020. (MIKAELA MACKENZIE / WINNIPEG FREE PRESS)
Dr. Edward Buchel, the head of surgeries at HSC, has seen firsthand how the high case numbers are impacting care in other parts of the province. Non-essential surgeries have been cancelled throughout the province’s two lockdowns and will continue to be cancelled as staff are moved to help COVID-19 patients.
“There's nothing more the hospital system can do,” he said. “We keep on transferring resources to keep people alive. The more it spreads, the more people will be in the hospital, the more we will shut down surgery. It's a simple equation.”
Buchel said people need to follow the public health orders to give the health-care system a chance to sustain itself, and potentially begin ramping up surgeries again in 2021.
“Don't spread the disease, wear your mask, don't socialize with people outside of your family, follow the public health rules,” he said. “They work. We know they work, they worked the first time.
“We're getting tired. Everybody doesn't follow them now, because they're getting tired. It is vital for the next six months that we follow these rules.”

Dr. Jazz Atwal, the acting deputy chief provincial public health officer for Manitoba, answers a question at a COVID-19 briefing on Dec. 16, 2020. (CTV News Photo Glenn Pismenny)
PREPARING FOR THE FUTURE
The COVID-19 pandemic is the first major worldwide pandemic of the 21st century that hit Manitoba, and will no doubt influence future health-care planning.
But what that influence will be is still not yet known.
Dr. Jazz Atwal, the acting deputy provincial public health officer, said each day of the pandemic is a learning process for public health.
“I think for the last couple of generations here at a minimum, everything we're doing is new to everyone,” he said on Dec. 16.
Atwal noted there will be time to reflect and look back on what the province can learn from the COVID-19 pandemic for future pandemics and identify gaps in care.
“But that will be far down the road, to be quite frank,” he said.
Lanette Siragusa, Shared Health’s chief nursing officer, said they will be working on their processes and developing plans should COVID-19 stick around, even with a vaccine approved.
“We're going to continue down the path we're on, and we're going to be diligent on making sure that all the processes and the supports are in place so that we can continue because I certainly don't feel like we're out of the woods yet with our hospital admissions and our ICU capacity.
“So for now it's status quo and we'll follow the numbers and follow the science and adjust as we need to in the future.”
This is the final installment in a three-part series 'Red Zone: On the front line of Manitoba's COVID-19 pandemic' from CTV News giving Manitobans a deeper look at the impacts of the COVID-19 pandemic on our health-care system. You can read the entire series by visiting our CTV News 'Red Zone' page.





































